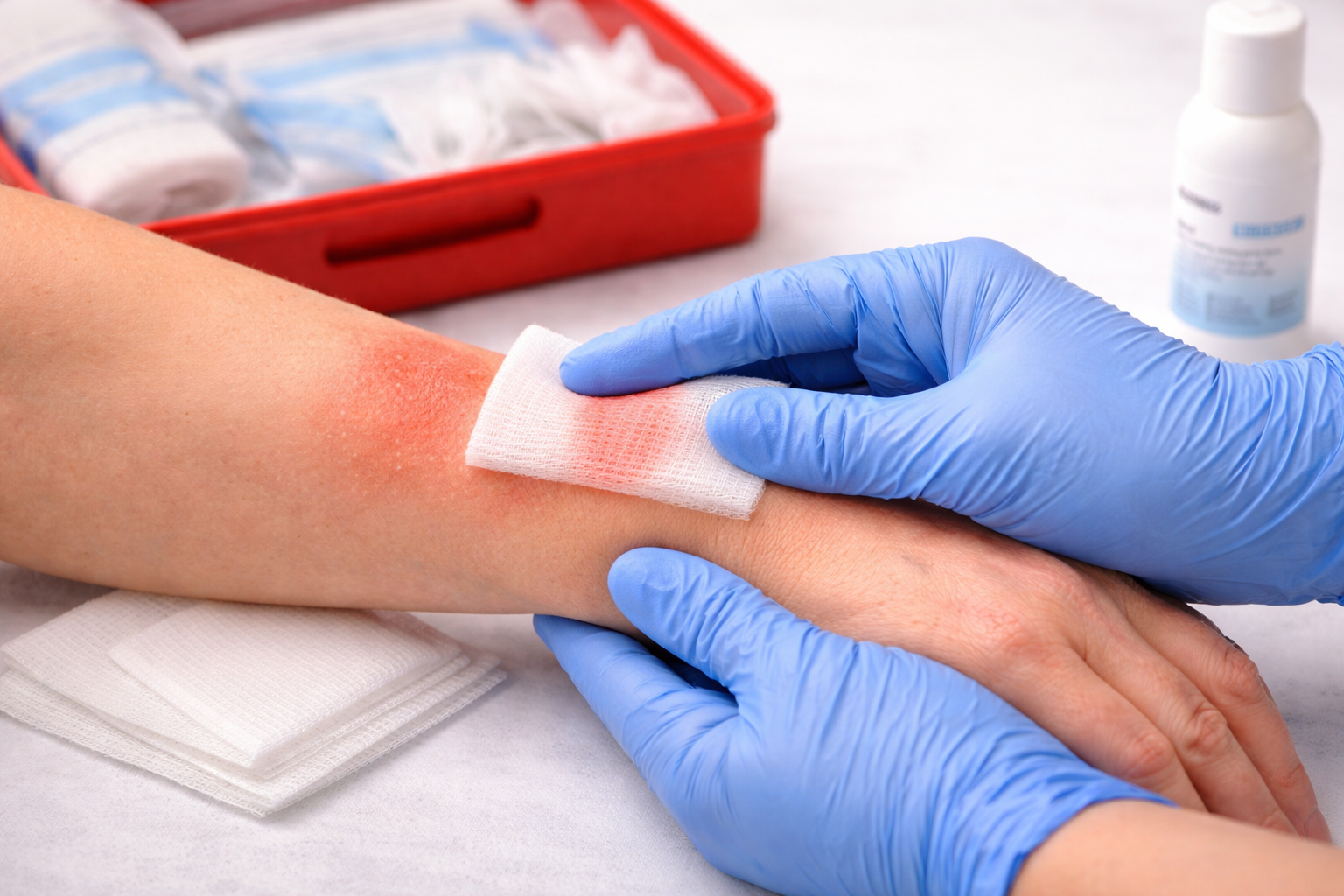
Introduction: Why Minor Burn Preparedness Matters More Than Most Workplace Goals
People want to eat better, exercise more, or save money, but without a clear plan and tools, those goals fade fast. The same pattern shows up in safety programs that claim to know how to treat minor burns, yet have no real system behind the promise.
Many workplaces already have a policy tucked into a binder that explains how to treat a minor burn. On the floor, though, responders often find half-stocked kits, unclear steps, and no agreement on when to handle a burn onsite versus send someone to urgent care. In kitchens, production lines, labs, clinics, and maintenance shops, small burns are common, and this gap between policy and practice shows up in real injuries.
Minor burns in a workplace usually mean first degree burns or very small, superficial second degree burns. Even when they look simple, poor care can lead to infection, lost work time, OSHA recordables, and workers’ compensation claims. Repeated bad experiences also erode staff trust in the safety program.
This guide walks through a practical, evidence-based process for how to treat minor burns in the workplace, step by step. It explains how to tell a true minor burn from a serious one, covers special cases like hands, lips, and steam burns, and shows how to build a standard protocol and supply plan. Along the way, you will see how a medical supplies and consumables partner, such as First Aid Longs, can help standardize kits and materials across sites with consistent quality and cost control.
Key Takeaways
A minor burn in workplace settings is usually a first degree burn or a very small, superficial second degree burn that is smaller than the worker’s palm and not on the face, hands, feet, genitals, buttocks, or major joints. Staff should treat anything larger, deeper, or in sensitive areas as more serious and escalate promptly.
The core first aid sequence for how to treat minor burns is simple and repeatable:
Stop the burning source
Cool the area with cool running water
Remove tight items
Gently clean
Apply appropriate topical care
Cover when needed
Monitor and document
Certain warning signs mean a burn is not minor and should bypass onsite care. These include burns larger than three inches, charring or white leathery skin, burns from electricity or strong chemicals, trouble breathing, signs of shock, or injuries in very young, older, or medically fragile people.
Facilities should spell out clear “do not” rules in posters and kits. Staff should not put ice directly on burns, use butter or oil, apply toothpaste or home remedies, pop blisters, or pull off clothing that is stuck to burned skin. These mistakes can worsen damage and increase infection risk.
Ongoing monitoring, simple infection checks, and awareness of tetanus status matter as much as the first few minutes. Daily dressing changes, watching for redness or pus, and a low threshold for medical review keep small burns from turning into larger clinical problems.
Procurement and safety teams can improve outcomes by standardizing minor burn protocols, aligning first aid stations with those steps, training staff, and maintaining dependable supply chains. Partners such as First Aid Longs support this work by providing consistent, high quality medical supplies and consumables with flexible manufacturing, OEM or ODM options, and on-time delivery across many sites.
What Counts As A Minor Burn In The Workplace
For safety officers and health coordinators, the first question is not how to treat minor burns, but whether the burn is truly minor. A minor burn in most workplaces is either a first degree burn or a very small, superficial partial thickness burn. These injuries are painful but shallow and cover a limited area.
In simple terms, first degree burns affect only the top layer of skin. The area looks red, feels sore, may be a little swollen, and has no blisters at first. A classic example is a quick touch of a hot pan or a mild sunburn on a construction worker’s neck. Superficial second degree burns go a bit deeper and may form small blisters, but if they are small and not on high risk body parts, they can still count as minor.
Size and location guide your decision more than anything else. If the burned area is smaller than the worker’s palm or about three inches across, and not on the face, hands, feet, genitals, buttocks, or a major joint, onsite care is usually reasonable. Burns from electricity or strong chemicals, however, are treated as serious until a clinician proves otherwise, even when they look mild on the surface. Vulnerable groups such as children, older adults, and people with major medical problems also deserve a lower threshold for referral. Written SOPs, wall charts, and kit inserts should spell out these rules in plain language.
A simple reference table can help frontline staff decide what can stay onsite and what must go out for higher care.
| Burn Feature | Likely Minor And Onsite | Needs Urgent Or Emergency Care |
|---|---|---|
| Red, dry, painful skin | Often yes | If a large area or a sensitive site |
| Small, clear blisters | Yes, if small and not on high risk area | Yes, if large, on the face, hands, feet, or genitals |
| Size smaller than worker’s palm | Often yes | Sometimes, no if mechanism is high risk |
| Electrical or strong chemical cause | Rarely | Almost always |
Superficial Vs Partial-Thickness: How To Recognize Minor Skin Burns
Understanding depth helps staff decide how to treat a minor burn on the skin and when to escalate. A superficial or first degree burn stays in the top layer of skin. It shows as flat redness, feels sore to touch, and may have slight swelling but no blisters at first. Brief contact with a hot tray, a curling iron in a locker room, or mild sun on a lifeguard’s shoulders are common examples.
Superficial partial thickness burns extend into the upper dermis. They look red or pink, often moist or shiny, and form small blisters. These burns usually hurt a lot, yet if the area is small and not on a high risk site, they often heal well with careful first aid. First degree burns tend to clear within three to seven days, while small partial thickness burns may take one to three weeks.
Pain level alone does not tell the whole story. Deep burns can damage nerves and may hurt less even when the tissue is badly injured. That is why any patch that looks pale, white, brown, or black, or feels numb instead of sore, should move immediately into the “not minor” category, no matter how small it appears.
When A Burn Is Not Minor: Escalation Criteria For Safety Teams
Safety teams need clear rules for when to skip onsite care and send the person straight to urgent or emergency care. A burn is not minor when it is larger than the worker’s palm, wraps all the way around a limb, or sits on the face, hands, feet, genitals, buttocks, or any major joint. Even a small blister across several knuckles can affect function and should be reviewed by a clinician.
Certain appearances are also red flags. Skin that is charred, white, brown, or leathery, with little or no pain in the worst areas, points toward deeper injury. Burns from electrical contact, lightning, or strong acids and alkalis are dangerous even when the surface looks like a simple first degree burn. Smoke or steam inhalation, hoarseness, soot around the nose or mouth, or any trouble breathing are clear reasons to activate emergency medical services.
Systemic signs matter as well. Cool clammy skin, rapid weak pulse, confusion, or sudden swelling near the burn can signal shock or airway risk. In hospitals, schools, and long term care, even apparently small burns in infants, frail older adults, or people with diabetes or immune problems deserve prompt evaluation. These criteria should appear on burn station signage, in training decks, and in procurement documents so that expectations match across departments and shifts.
Step-By-Step: How To Treat Minor Burns In The Workplace
Once a burn meets minor criteria, staff can follow a standard process for how to treat minor burns in the workplace. This process lines up with guidance from groups such as the American Burn Association and the American Academy of Dermatology. It works for minor thermal burns from hot surfaces, brief flames, hot water, steam, and many kitchen incidents. Chemical and electrical burns still follow special escalation rules even if they seem small.
For safety, compliance, and workers’ compensation, it helps to document each step with time stamps and products used. Procurement teams can map each stage to medical supplies and consumables so that first aid stations always support the protocol. The steps below can be turned into SOPs, wall posters, and quick training aids across plants, clinics, and offices.
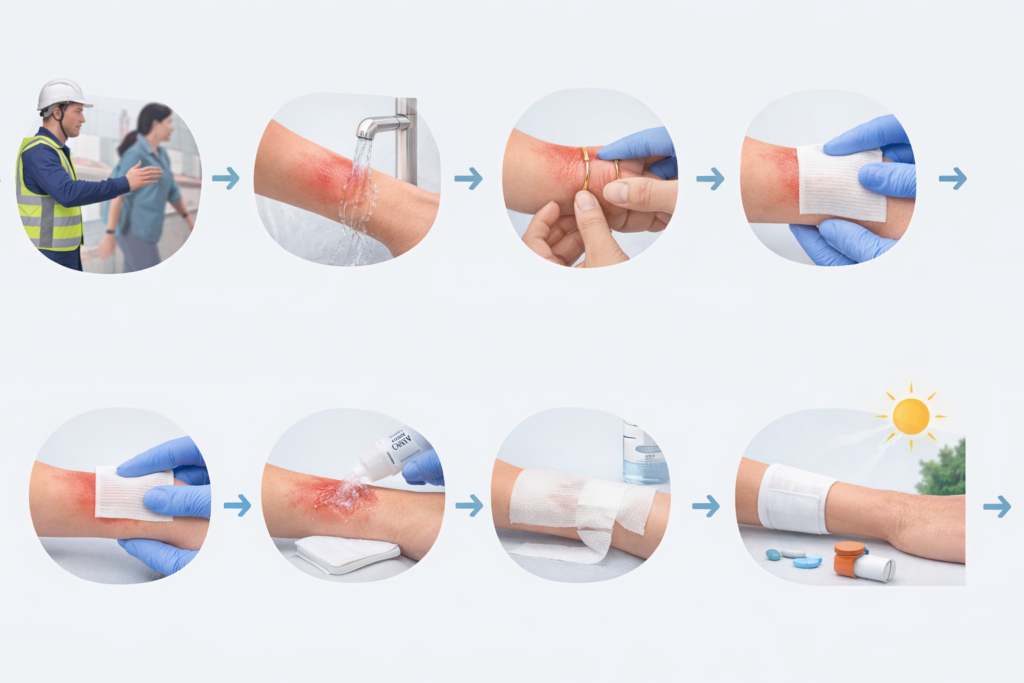
Step 1: Stop The Burning Process And Ensure Scene Safety
The very first action is to stop the heat source and make the area safe. Turn off or move away from hot equipment, flames, boiling liquids, or steam vents. In kitchens or lab spaces, guide the injured person out of the spill or splash zone before doing anything else.
Responders should protect themselves with gloves and, in splash risk areas, eye protection. With suspected electrical burns, power must be shut off or locked out before anyone touches the victim. If clothing near the burn is not stuck, it can be cut away with bandage scissors to expose the area, but fabric that has melted into the skin should be left in place for medical staff. Recording how the burn happened helps both clinical review and future prevention work.
To keep this step consistent, many sites:
Add quick reminders on burn station posters
Include “stop the source first” in first aid drills
Require brief incident notes right after care
Step 2: Cool The Burn Correctly (No Ice)
Cooling is the most time sensitive part of how to treat a minor burn and often makes the biggest difference in outcome. For most minor thermal burns, place the area under cool, not cold, running tap water for at least five to ten minutes, or until pain eases. On a production line or in a busy kitchen, supervisors should be ready to free the worker from the task so that this cooling can happen right away.
If running water is not available, use a clean, cool, wet cloth and rewet it often to keep the area comfortable. For minor burns inside the mouth from hot drinks in a cafeteria, cool water sips or small ice chips that melt slowly can help, as long as the person can swallow safely. Staff should avoid placing ice or very cold packs directly on the burn, since this can narrow blood vessels and damage tissue. Very long immersion in cold water, especially for larger areas or fragile workers, should also be avoided.
From a planning view, high risk zones need nearby sinks or emergency eyewash style fixtures with tepid water. Where that is not possible, facilities may stock sterile saline bottles and clear instructions that cooling with water comes first before any gel or dressing.
Step 3: Remove Rings, Watches, And Tight Items Early
After cooling begins and the person is away from danger, attention shifts to items that can trap swelling. Burns often lead to rapid puffiness, especially in fingers, hands, and arms. Rings, watches, bracelets, tight sleeves, or fitness bands can quickly become a problem and cut off circulation.
Responders should remove these items gently and as early as possible, before the area swells. If a ring or bracelet will not come off easily, do not waste long minutes or cause more pain; note the problem and send the person for medical care. Clothing that is burned into the skin should never be torn away. Trauma shears in first aid stations make it easier to cut around safe areas without pulling on damaged tissue. Documenting which items were removed and when can assist clinical staff later if questions come up.
Step 4: Gently Clean And Assess The Burn
Once the burn is cooled and constricting items are off, the next step in how to treat minor skin burns is gentle cleaning and assessment. For first degree burns with unbroken skin, simple rinsing with clean water followed by careful drying with a lint free cloth is usually enough. There is no need to scrub, and harsh products can delay healing.
For small superficial partial thickness burns, responders can rinse with water or saline if the area is not heavily contaminated. Intact blisters should be left alone because they act like the body’s own bandage. Cleaning focuses on the surrounding skin, not on scrubbing the blister itself. After this rinse, staff should look again at size, depth, and location to confirm that onsite care is still appropriate. Any sign that the burn is deeper or larger than first thought should trigger escalation.
Step 5: Apply Appropriate Topical Products For Minor Skin Burns
With the area clean, responders can think about comfort and healing products. For many first degree burns, a thin layer of plain petroleum jelly applied two or three times per day keeps the skin moist and reduces dryness and cracking. Products that contain aloe vera and are designed for skin use can also soothe small burns, as long as they are fragrance free and alcohol free.
Thick layers of greasy ointments or strong antiseptics are not helpful in simple, clean first degree burns. Topical antibiotics may be considered only if a small blister breaks open and a clinician or occupational health provider recommends them. Workplaces should clearly ban butter, cooking oil, toothpaste, egg whites, and other home remedies from their first aid practice. One key rule for how to treat minor burns at home also applies at work, which is to wait until cooling is complete before putting any ointment or gel on the area. Procurement teams often favor single use packets of approved products, which lowers the risk of contamination from shared jars and tubes.
Step 6: Cover And Protect The Burn
Covering a burn can cut pain and protect against dirt and friction. Some very mild sunburns or flat first degree burns on low friction areas can stay open to the air with regular moisturizing. But in most workplaces, areas that rub against clothing or contact tools, such as hands and forearms, benefit from protective bandaging.
The best choice for minor burns is a sterile, non stick pad placed gently over the area. For blisters or open spots, this keeps the surface moist but not soggy and prevents the dressing from pulling off new skin. Gauze wraps or soft cohesive bandages can hold the pad in place, but they must be applied loosely so circulation stays normal. Staff should change dressings at least daily, or sooner if they get wet or dirty, using clean technique and gloves each time. Fingers and thumbs may need special finger wraps or tubular gauze that protect the area while still allowing some movement.
To support this step, many organizations standardize:
Non stick pads in several sizes
Soft gauze rolls and cohesive wraps
Gloves and small tape rolls at every first aid point
Step 7: Manage Pain, Hydration, And Comfort
Minor burns often hurt more than they look. Part of how to treat a minor burn is helping the person stay comfortable enough to work safely or rest as ordered. Over the counter pain relievers such as acetaminophen or ibuprofen are common choices, but workplaces must follow their own medical policies and local rules. In many settings, only occupational health staff or nurses can give these medicines, and every dose must be logged.
Hydration matters too, especially after a minor kitchen burn, a steam burn in a boiler room, or a sunburn on an outdoor crew. Encouraging water or appropriate electrolyte drinks helps the body recover from both heat and burn stress. When possible, elevating a burned arm or leg above heart level reduces swelling and throbbing. Supervisors may need to adjust duties for a short period if bandages affect grip strength or if pain would make certain tasks unsafe.
Step 8: Protect Healing Skin From Sun And Irritants
Once the skin has closed and there are no open areas, attention shifts to long term skin health and scarring. New skin is thin and sensitive. Direct sun can darken or redden the area, especially on the face, neck, forearms, and hands, leading to longer lasting marks. For workers who spend time outdoors, a broad spectrum sunscreen with SPF thirty or higher and protective clothing such as long sleeves, gloves, and hats is very helpful.
Irritants also slow healing. Staff should keep solvents, strong cleaners, and abrasive materials away from the area while it recovers. Light moisturizing with gentle creams helps the new skin stay flexible. This is especially important for people who ask how to treat minor burn scars and want the best cosmetic result. Post burn care guidance can be built into discharge instructions from occupational health or urgent care, so workers know what to do at home as well.
Special Scenarios: How To Treat Minor Burns On Hands, Face, And In High-Risk Tasks
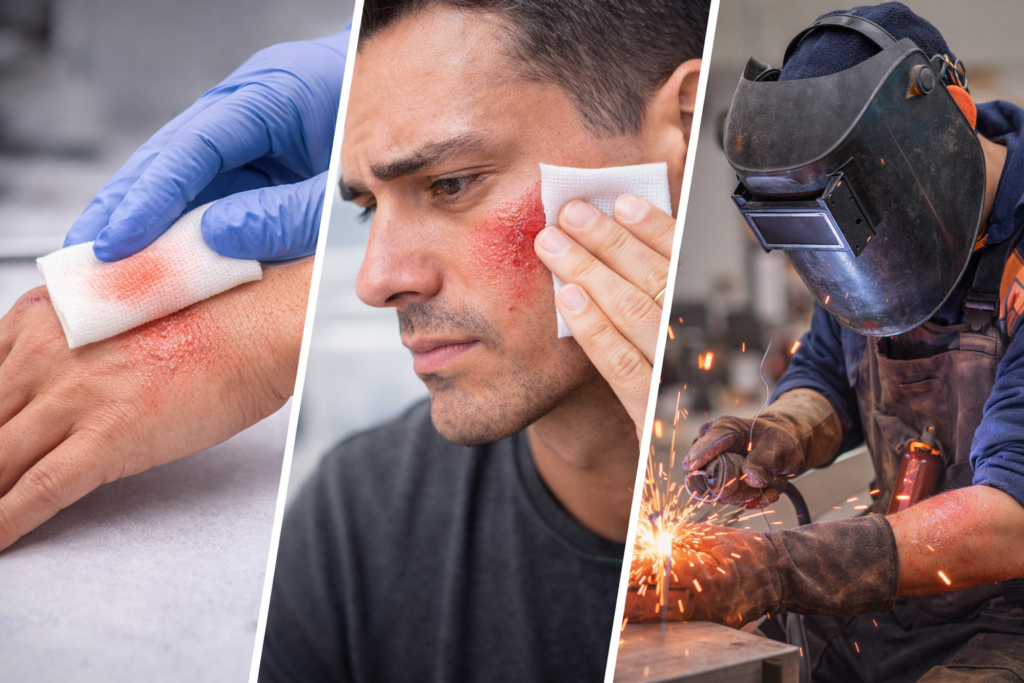
Not all minor burns carry the same impact. A small blister on the upper arm is very different from the same blister on the fingertip of a machinist or the lip of a teacher. Safety teams often field detailed questions such as how to treat a minor burn on the hand, how to treat a minor burn on the face, or how to manage a small splash from hot oil in a busy kitchen.
The good news is that the core sequence for how to treat minor burns still applies in these special cases. The difference lies in how you cool, dress, and monitor the area, as well as when you decide that function or appearance concerns call for medical review. Scenario based training and quick reference cards can help supervisors apply the general rules to these specific situations.
How To Treat A Minor Burn On Finger, Hand, Thumb, Or Arm
Hands and arms are among the most common sites for workplace burns. For how to treat a minor burn on a finger or how to treat a minor burn on a thumb, place the hand under cool running water with fingers spread so every surface gets cooled. Early removal of rings and watches is especially important here, since swelling in the digits can become dangerous very fast.
After cooling and cleaning, a thin layer of petroleum jelly plus a small non stick pad often works well. Tubular gauze or purpose made finger bandages can protect the area while keeping joints mobile. Similar steps apply to how to treat a minor burn on the hand or how to treat a minor burn on the arm, with special care not to wrap bandages too tightly. Even small burns on hands may need medical review if blisters cross joints, if several fingers are involved, or if pain makes it hard to grip tools or type. Temporary duty changes can keep injured staff safer while healing.
How To Treat Minor Burns On Face, Lip, Or Near Joints
When staff ask how to treat a minor burn on the face or how to treat a minor burn on the lip, the answer starts with gentle cooling. Cool, damp cloths work better than immersion, and care must be taken to avoid water in the eyes. Any burn that affects eyelids, eyeballs, or the inside of the mouth should prompt immediate medical attention, even if it seems small.
For truly superficial facial burns, light cooling followed by thin layers of petroleum jelly or an approved moisturizer may be enough. On the lips, mild burns from hot drinks can be cooled with water or ice chips and then kept moist with simple, fragrance free balms. Burns around joints such as wrists, elbows, or knees raise extra concern, since scarring could limit motion. These areas should be dressed in ways that protect the skin while still allowing gentle movement, and any sign of stiffness or pain with motion is a reason to call a clinician.
How To Treat Minor Kitchen, Steam, Hot Water, And Oil Burns At Work
Food service, hospitality, and healthcare kitchens see frequent questions about how to treat a minor kitchen burn and how to treat a minor burn from hot water. The sequence still starts with moving away from the source, cooling with running water, removing tight items, cleaning, and dressing. Steam burns often affect scattered spots on hands and arms, so responders need to inspect all exposed skin and cool every area that looks red or feels sore.
Oil burns bring extra heat because hot fat clings to the skin. For how to treat minor oil burns or how to treat minor burns from cooking, longer, gentle cooling with water is key. Thick layers of burn gel without prior cooling can trap heat, so staff should always cool first, then consider soothing products. Small steam burns and hot water splashes that cause tiny blisters can often be handled onsite with non stick dressings. Any burns that involve deep fryer spills, large areas, or the face require urgent medical care. Prevention efforts such as non slip mats, heat resistant gloves, and safe carrying rules for hot liquids reduce these incidents over time.
How To Handle Suspected Minor Chemical Or Electrical Burns
Questions around how to treat a minor chemical burn or how to treat a minor electrical burn demand a cautious answer. In many cases, these burns are not minor at all, even if the skin looks only slightly red. For chemical exposure, the immediate step is long, generous rinsing with water, often for twenty minutes or more, following the product’s Safety Data Sheet. Contaminated clothing and PPE should come off carefully while rinsing continues.
Because chemicals can keep damaging tissue and electrical currents can injure deeper structures and the heart, most facilities treat these mechanisms as automatic reasons for medical review. At most, very small splashes of low risk chemicals on skin that look like simple first degree burns may be managed like other minor burns, but even these cases should be checked by occupational health. Protocols should state that almost all electrical and chemical burns move off-site quickly, rather than encouraging staff to guess about depth.
Building A Standardized Minor Burn Protocol And Supply Plan
Even the best clinical advice on how to treat minor burns will fail if each site responds in a different way. Unplanned care leads to uneven outcomes, confusion in an emergency, and wasted money on mismatched supplies. A standardized protocol and supply plan turns burn response into a simple routine that any trained staff member can follow.
A written minor burn SOP should follow the evidence based steps already outlined, from initial safety check to follow up and documentation. Procurement teams can then translate each stage into medical supplies and consumables, such as cooling and cleansing materials, dressings, gloves, and documentation tools. Partners like First Aid Longs, with in house manufacturing, 100K Class cleanroom facilities, and OEM or ODM services, can help organizations build consistent, high quality kits that match their protocols across multiple locations.

Core Elements Of A Workplace Minor Burn SOP
A good SOP for how to treat minor burns first aid reads like a simple flow rather than a dense manual. It starts with a quick classification, asking about size, depth, location, and cause to separate minor burns from major ones. Next, it outlines the exact steps for stopping the heat source, cooling with water, removing rings and tight items, cleaning, applying topical products, bandaging, and supporting comfort.
At each step, the SOP notes who is allowed to act. It clarifies which staff can give medicines, who can approve transport to urgent care or emergency departments, and who completes incident forms. It also links actions to OSHA reporting and workers’ compensation processes, so records are complete. Visual versions of this SOP, such as posters near first aid stations or laminated cards for supervisors, help keep the process front of mind during real incidents.
For clarity, many SOPs include a one-page flow chart that:
Starts with “Is the burn minor?” checks
Splits into onsite care vs escalate now paths
List supplies needed at each step
Aligning First Aid Stations, Kits, And Supplies With The Protocol
Protocols only work when supplies match the plan. For how to treat minor burns on the hand, for example, responders need non stick pads, tubular gauze, gloves, and tape right at the station, not across the building. Procurement teams can map each step of the SOP to a supply category, from cool running water access and cleansing materials to petroleum jelly packets, aloe based gels, dressings, wraps, and documentation forms.
Standardizing kit layouts and contents across all sites makes training and restocking much easier. High risk zones such as kitchens, machine shops, boiler rooms, and labs may need larger burn-focused kits with more dressings and gloves. Regular audits and expiry checks keep supplies usable. With its cleanroom production, low minimum order quantities, and experience serving more than one hundred global clients, First Aid Longs can support consistent, cost-efficient stocking of the medical supplies and consumables that burn protocols depend on.
A simple burn kit checklist often includes:
Cool water access or sterile saline
Non stick dressings and gauze
Petroleum jelly or approved burn gels
Disposable gloves and trauma shears
Incident report forms or digital logging tools
Training, Drills, And Continuous Improvement
Even a well-written SOP and well-stocked kits will gather dust without training. Supervisors, designated first aiders, and clinical staff need regular practice in how to treat minor burns, at least once a year and when protocols change. Scenario-based drills using likely events, such as hot water splashes in a cafeteria, contact burns from equipment in a plant, or mild chemical splashes in a lab, help staff apply the steps under pressure.
Incident and near-miss reports are valuable data points. Safety and procurement leaders can review them together to spot patterns, such as frequent finger burns at a certain station or recurring questions about how to treat minor burn blisters. These reviews may point to better PPE, equipment changes, or updates to training. Documenting all training sessions also supports regulatory and accreditation needs and proves that the organization takes burn care seriously.
Secure Reliable Burn Gel Supplies Today!
Order our high-quality wholesale burn gels made with safety standards to stabilize your healthcare operations.

Conclusion
Minor burns are common in healthcare facilities, factories, construction sites, kitchens, and offices, yet they do not have to create major problems. Clear rules about what counts as a minor burn, based on depth, size, location, and cause, help staff decide when onsite care is safe and when escalation is needed. From there, the same straightforward steps for how to treat minor burns apply almost everywhere.
Stopping the heat source, cooling with water, removing tight items, cleaning gently, choosing the right topical products, covering with non-stick dressings, and supporting comfort form a simple, reliable pattern. When organizations add infection checks, awareness of tetanus status, and clear escalation points, they greatly reduce the chances that a small burn will turn into a bigger medical or legal issue.
Operationally, a strong minor burn program pays off in fewer complications, less downtime, higher worker confidence, and a better compliance posture. The key is to connect protocols, training, and supply planning instead of treating each burn as a one-off event. Standard first aid stations, consistent kits, and realistic drills make the process easy to follow on the worst day, not just on paper.
For procurement managers, safety officers, and clinical leaders, partners such as First Aid Longs play an important role. With comprehensive in-house manufacturing, 100K Class cleanroom facilities, flexible OEM and ODM services, low minimum order quantities, and dependable delivery, First Aid Longs helps organizations source medical supplies and consumables that match their burn protocols across many sites. When every location follows the same evidence based steps with the same high quality materials, minor burns stay minor, and the safety program moves from good intentions to everyday practice.